Analysis shows low energy diets with formula meal replacements are the most effective methods for weight management and remission in adults with type 2 diabetes
A new study published in Diabetologia (the journal of the European Association for the Study of Diabetes (EASD) finds that low energy diets with formula meal replacements are the most effective methods of weight management and remission in adults with type 2 diabetes (T2D), while the macronutrient content is not important to outcomes.
The research was conducted by Professor Mike Lean, Dr Chaitong Churuangsuk and colleagues at the Universities of Glasgow, (with Dr Churuangsuk also affiliated to Prince of Songkla University, Hat Yai, Thailand) and others from Cambridge (UK) and Otago (New Zealand) Universities. The group analysed published meta-analyses of which type of diet is best for achieving and then maintaining weight loss in adults with T2D.
While T2D is influenced by both genetic and environmental factors, it is rising levels of overweight and obesity which have driven the current global epidemic of diabetes. The authors note: “Without strategic commitment internationally on effective prevention strategies, type 2 diabetes will affect an estimated 629 million people worldwide by 2045.”
The onset of T2D is primarily driven by weight gain to the point that it becomes unhealthy. The amount of weight-gain needed varies widely between individuals. The development of the disease involves a complex interaction of gut hormones, low-grade inflammation and possibly metabolites from the gut microbiota. It develops in susceptible individuals and families who tend to have large waists and who accumulate fat in their liver, pancreas and muscles. This impairs organ functions, resulting in hyperglycaemia (abnormally high blood sugar), commonly associated with hypertension (high blood pressure) and abnormal blood fats.
T2D requires lifelong management, but even with treatment it can cause disabling, painful and life-shortening complications. However, sufficient weight loss can remove the abnormal body fat from liver and pancreas and reverse diabetes.
Weight loss is critical to management and remission of T2D and has been shown to improve all the related cardiometabolic risk factors and reduce the patient’s need for medication.
In the UK DiRECT study, funded by Diabetes UK, almost 80% of people with T2D for up to 6 years who lost over 10kg, and maintained the weight loss of over 10 kg, remained in remission from diabetes for at least 2 years.
While there is widespread awareness of the benefits of weight loss for people withT2D, there is a lack of authoritative guidance over dietary advice, to inform both patients and healthcare providers. Ill-informed controversy over diet types has contributed to inaction and delays in providing effective treatment. Current guidelines stress the importance of personalised weight management and state that various diet strategies may be effective, but do not provide information about diet composition. This can lead to patients following diets based on distorted evidence and misleading claims.
Adherence to any energy-reduced diet will lead to sustained weight loss, provided that energy (calorie) use exceeds intake. However, in practice, adherence rates and weight losses vary widely, even within the same diet programme, and some comparisons between diets appear to show conflicting results.
The researchers wanted to help resolve these uncertainties and to inform clinical decision making and guideline development, as part of a programme of work to update the recommendations of the European Association for the Study of Diabetes (EASD).
For this new study, the researchers collected and systematically reviewed all the relevant world publications of diet trial meta-analyses for weight management of people with T2D, and all studies which have reported remissions of T2D.
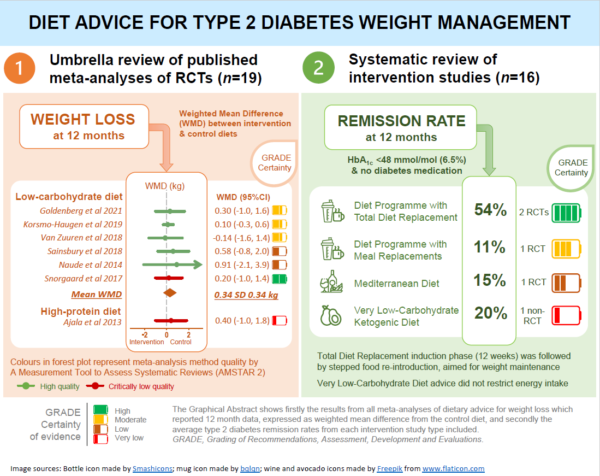
Their analysis found that the greatest weight loss was achieved with very low energy formula diets, used as ‘Total Diet Replacement’ at 1.7-2.1 MJ/day [400-500 kcal/day] for 8-12 weeks, which led to an average 6.6kg more weight lost compared to food-based low-energy diets (4.2-6.3 MJ/day [1000-1500 kcal/day]). Formula meal replacements were also found to be superior to food-based low-energy diets alone, achieving 2.4kg greater weight loss over 12-52 weeks.
The published evidence showed that low-carbohydrate diets were no better than higher carbohydrate (low-fat) diets for weight loss.
For remission of T2D, there are no direct comparisons between diet types, but published studies showed the best remission rates of 46-61% at 12 months with programmes that include a formula ‘Total Diet Replacement’ of 830 kcal/day for 12 weeks, followed by a relatively low-fat high carbohydrate diet and meal replacements for long-term maintenance. With low carbohydrate diets, reported remission rates are much lower at 4%-19% of those who tried the diet.
They add: “Mediterranean, high-monounsaturated-fatty-acid, vegetarian and low-glycaemic-index diets all achieved minimal (0.3-2 kg) or no difference from conventional relatively low fat/high carb control diets…The evidence, albeit of variable quality, is rather consistent showing that no one diet type is superior over others for weight management in type 2 diabetes.”
The researchers conclude: “Published meta-analyses of diets for weight management in people with type 2 diabetes do not support recommending any particular macronutrient profile or style over others. Very low energy diets and formula meal replacement appear the most effective approaches, generally providing less energy than self-administered food-based diets.”
A limitation of the trials examined by this study is that the benefits from weight management depend largely on long-term control of body weight, while most of the currently available evidence relates only to short-term outcomes. Successful long-term maintenance of weight may require different behavioural strategies to those effective for the weight-loss phase. Few trials have reported data beyond 12 months. The team suggest: “Well-conducted research is needed to assess longer-term impacts on weight, blood sugar control, clinical outcomes and diabetes complications.”
Professor Lean adds: “anyone who is marketing a programme for weight loss or remission of type 2 diabetes should declare all the results
All News